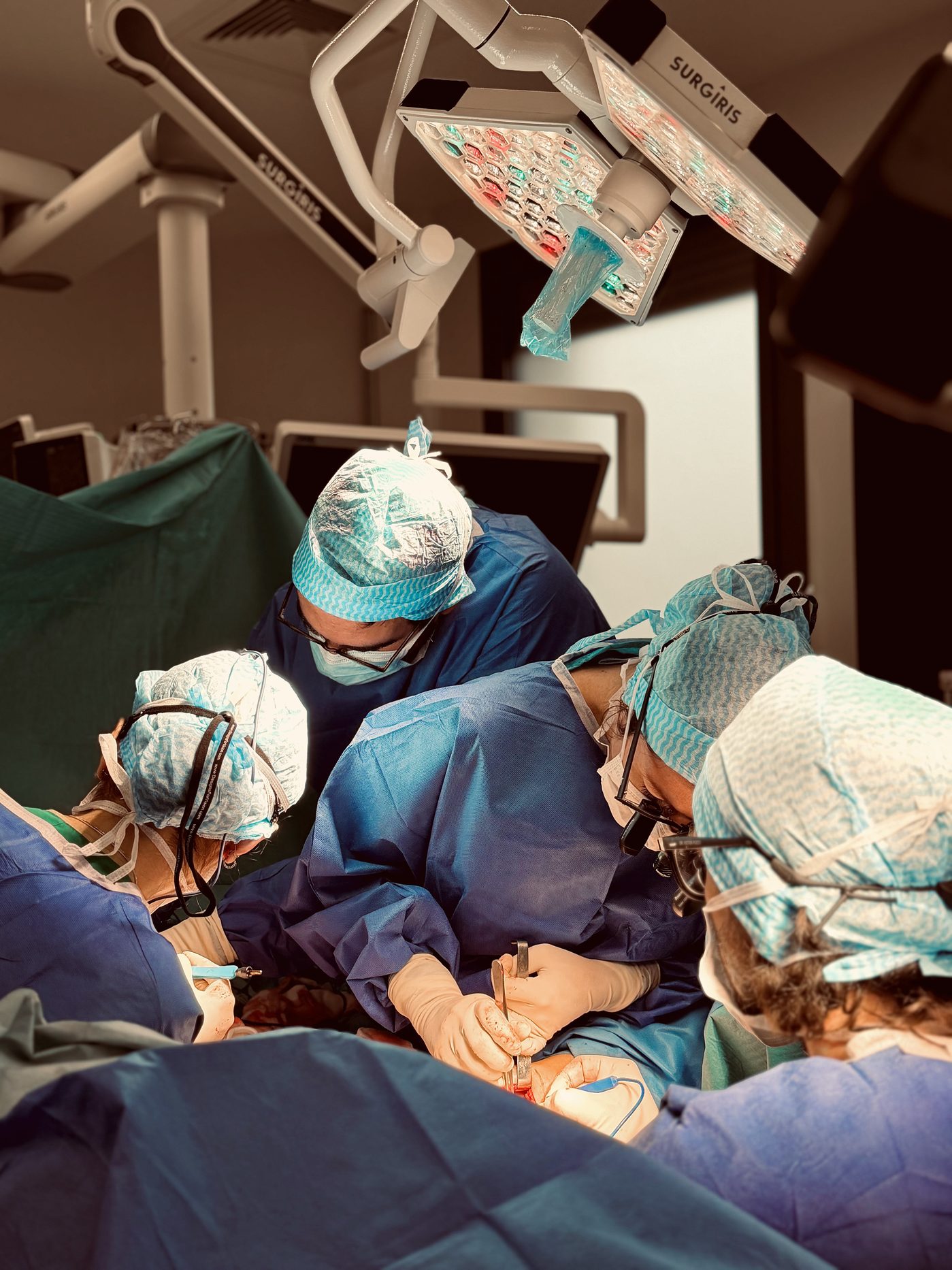
The procedure involves harvesting a horizontal ellipse of skin and fat from the upper inner thigh. Two variants exist. The gracilis flap (TMG — transverse myocutaneous gracilis flap — or TUG — transverse upper gracilis flap), described in 2004, takes a small accessory muscle, the gracilis muscle, along with the cutaneous-fat paddle. The PAP flap (Profunda Artery Perforator), described in 2012, takes only a pure cutaneous-fat paddle, without any muscle.
In both cases, the flap is transferred to the chest. Its vessels are reconnected under a microscope to vessels of the axilla or chest, behind the third or fourth rib: this microsurgical step keeps the tissue alive. Dr Zeitoun does not perform microsurgery himself — this part of the procedure is carried out in close collaboration with an experienced plastic microsurgeon.
The flap is then shaped to give it the natural conical form of a breast. The volume provided is moderate — a second stage with autologous fat transfer (lipomodelling) may be required to obtain a larger volume. The reconstruction is definitive and evolving: it follows weight fluctuations like a natural breast.
3–5 h
Operative time
A long procedure given the microsurgical time. The outcome is natural and durable — the flap evolves with the body like a natural breast.
100%
National health insurance base (ALD)
Procedure reimbursed based on the Sécurité Sociale tariff. Dr Zeitoun practises under sector 2 — additional fees apply. A written quote is provided before any surgery.
3–5 nights
Hospital stay
Hospital stay of 3 to 5 nights for microsurgical flap monitoring. Full recovery at least 4 weeks.