Understanding your
breast MRI
Who breast MRI is for, how the exam unfolds, how to read the report — a simple, step-by-step guide to understand what is being looked for, what is found, and what it means for you.
Who breast MRI is for, how the exam unfolds, how to read the report — a simple, step-by-step guide to understand what is being looked for, what is found, and what it means for you.

Breast MRI is not a routine exam. It is the most sensitive imaging tool available for the breast — used in specific situations where mammography and breast ultrasound are no longer enough.
Concretely, MRI stands for magnetic resonance imaging. No X-rays, no radiation: a powerful magnet and radio waves generate the images. It is a painless exam, but you need to remain still for around 30 minutes inside a tunnel.
For breast MRI to be fully informative, it is almost always performed with an injection of a contrast agent through an arm IV. This contrast highlights areas that are highly vascularized — typically cancers, which build their own network of small vessels to feed themselves. That is what gives MRI its precision.
One important point: if you are not menopausal, the exam will ideally be scheduled between day 7 and day 14 of your cycle. During that window, breast tissue is more "quiet" and the images are more reliable. The radiology center will ask the date of your last period before scheduling.
Unlike mammography, MRI is not a yearly screening exam for all women. It is prescribed in well-defined situations where it truly adds something on top of mammography and ultrasound.
For women at very high risk of breast cancer: BRCA1 or BRCA2 mutation, significant family history, other known mutations. MRI is then performed every year from age 30, alongside mammography and ultrasound.
When a breast cancer has just been diagnosed, MRI may be requested to map the exact extent of the tumour, look for additional lesions, and better plan surgery.
When mammography and ultrasound cannot resolve a doubtful area, MRI often allows a clearer view and guides next steps: surveillance, biopsy, or reassurance.
MRI is the reference exam to check the integrity of breast implants in case of doubt, and may be useful for follow-up after treated breast cancer, alongside routine mammography.
In all cases, MRI is prescribed by your physician (gynecologist, breast surgeon, radiologist) and covered by the French national health insurance in those indications. Without a clear indication, MRI is neither useful nor recommended — it can generate false alarms.
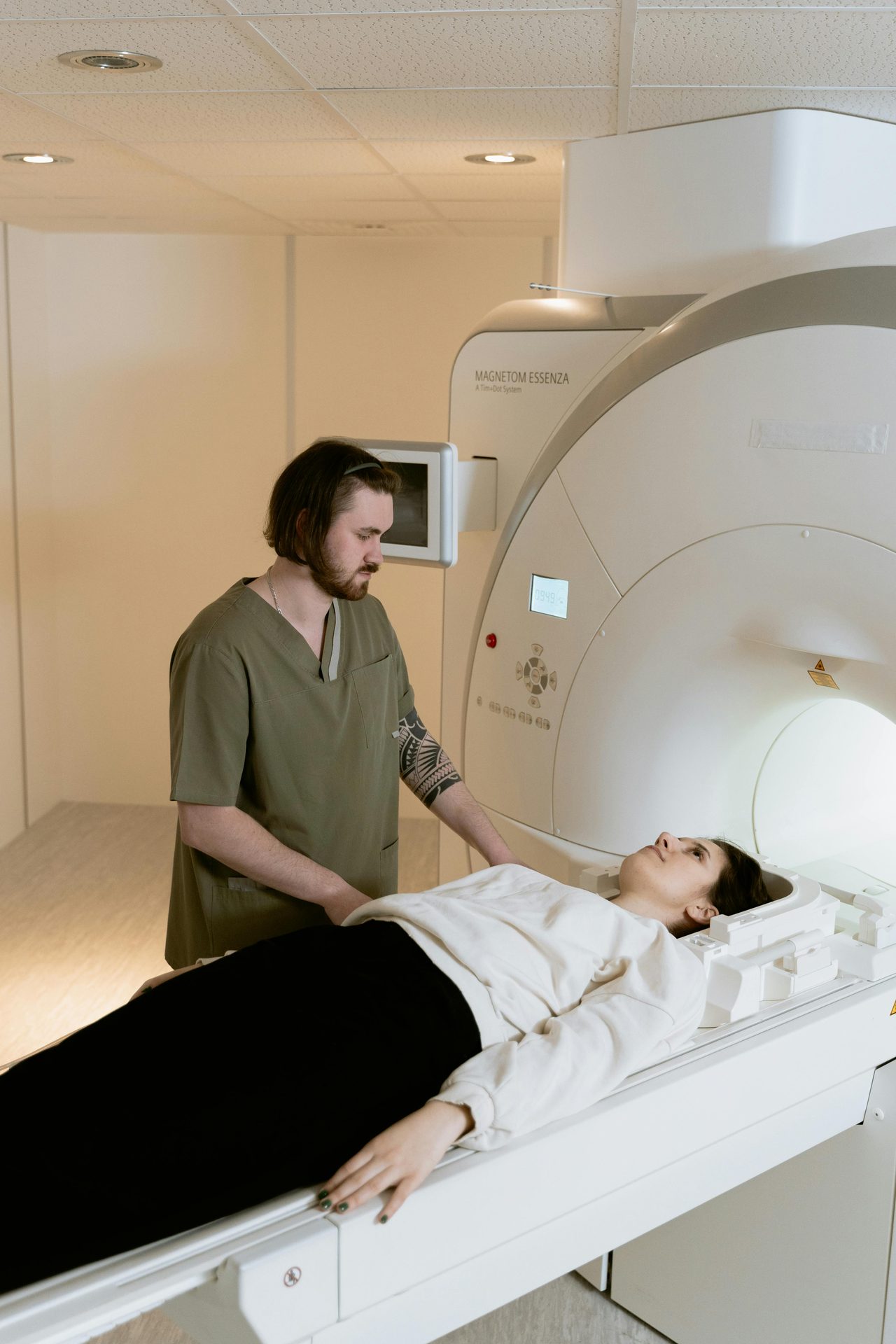
On arrival at the radiology center, you fill in a safety questionnaire — it checks for any contraindication to entering the machine (pacemaker, certain old metallic implants, certain metal foreign bodies). You remove all metal items: jewellery, underwire bra, watch.
An IV line is placed in your arm to inject the contrast agent during the exam. That is the only minor discomfort of breast MRI — everything else is completely painless.
You are then placed face down (prone position) on the table, with your breasts free in a dedicated coil. This position avoids compression and provides the best images. The table slides into the tunnel. The machine is loud, with intermittent mechanical knocking sounds — earplugs or headphones are provided. You hold an alert button in your hand to call the technologist at any time.
The exam takes around 30 minutes. During that time, several image series are acquired: before the injection, then during and after the contrast injection. That is why staying still matters: any movement degrades image quality.
At the end, the IV is removed, you can get dressed and leave. You don't need to be accompanied (unless you took an anxiolytic for claustrophobia). The images are available right away on a CD or digital platform. The radiologist's written report is generally available within 24 to 72 hours.
The radiologist reading your MRI mainly looks for areas that take up the contrast agent — this is called enhancement. When an area appears whiter after the injection, it is highly vascularized. That is where attention is focused.
On the report, you will mostly come across two terms:
A well-defined area taking up contrast — like a "ball" visible on the images. The radiologist analyses its shape (round, oval, irregular) and its margins (smooth = rather reassuring; blurred or irregular = more suspicious).
An area that takes up contrast without forming a clear ball. The radiologist then looks at how it is distributed in the breast — diffusely, along a duct, or across a whole segment — to decide whether it is suspicious.
Alongside this, the radiologist also notes the background parenchymal enhancement: how much normal breast tissue itself takes up some contrast diffusely. This varies between women and during the cycle — which is exactly why MRI is ideally scheduled in the second week of the cycle.
The BIRADS classification (Breast Imaging Reporting And Data System), used in France under the term ACR, is the universal language of radiologists. It is shared across mammography, ultrasound and MRI. Each exam ends with a 0–6 score that summarizes the level of suspicion and guides next steps.
Important: an ACR score is never read in isolation. It is always interpreted in context — your age, history, the precise appearance of the lesion, its evolution, and consistency with mammography and ultrasound. If anything in the report is unclear, talk to your physician or book a dedicated consultation.
Here are the next steps depending on the score.
No specific action. Continue routine surveillance based on your indication (annual for BRCA, ad-hoc otherwise). The next MRI is set by your physician.
If the lesion is also visible on ultrasound: targeted ultrasound recheck at 4 months. If visible only on MRI: MRI recheck at 4-6 months. Upfront biopsy possible if the patient is anxious.
If the lesion is also visible on ultrasound: ultrasound-guided biopsy at the office (the simplest). If only visible on MRI: MRI-guided biopsy, in dedicated radiology, under local anesthesia.
Depending on the situation, additional exams may be discussed: targeted ultrasound to look for the MRI lesion, targeted mammography to check for associated microcalcifications, or MRI-guided biopsy when the lesion is only visible on MRI. Your breast surgeon is here to guide you through every step.
Breast MRI is not a routine screening exam. It is indicated in specific situations:
— High-risk surveillance: BRCA1/2 mutation, significant family history, other known mutations. MRI is then performed annually from age 30, alongside mammography and ultrasound.
— Staging of newly diagnosed breast cancer: MRI maps the extent of the tumour and looks for additional lesions.
— Ambiguous finding not resolved by mammography and ultrasound.
— Suspected recurrence after treated cancer, when standard imaging is unclear.
— Implant integrity check when in doubt.
It is prescribed by your physician and covered by the French national health insurance for these indications.
The exam takes about 30 minutes. You fill in a safety questionnaire, remove all metal items, and an IV line is placed in your arm to inject the contrast agent during the exam.
You lie face down with your breasts free in a dedicated coil. The table slides into the tunnel. The machine is loud — earplugs or headphones are provided. You hold an alert button.
The exam is painless. At the end, the IV is removed and you can leave right away. The written report is available within 24 to 72 hours.
No, the exam is painless. No breast compression, unlike mammography. The only minor discomfort is the IV placement in your arm.
The machine noise can be unpleasant, but earplugs or headphones are provided.
The contrast agent is injected through an IV during the exam. It concentrates in highly vascularized areas — typically cancers, which build their own network of small vessels to feed themselves.
Without injection, breast MRI loses most of its diagnostic value. The agent used is not iodine-based (nothing to do with CT scan allergy) and is generally very well tolerated. True allergic reactions are exceptional. The main precaution concerns patients with known kidney impairment.
The ACR/BIRADS classification standardizes image interpretation. It is shared across mammography, ultrasound and MRI. Each exam ends with a score:
ACR 1: normal. ACR 2: clearly benign. ACR 3: probably benign — short-term recheck. ACR 4: suspicious — biopsy indicated. ACR 5: highly suggestive of cancer — biopsy mandatory. ACR 0: incomplete. ACR 6: cancer already proven.
An ACR 3 lesion on MRI has less than 2% cancer risk. Standard approach is close surveillance.
Timing depends on what is seen:
— If the lesion is also visible on ultrasound: recheck by targeted ultrasound at 4 months (simpler and faster than MRI).
— If the lesion is visible only on MRI: recheck by breast MRI at 4-6 months.
If the lesion is stable, it is reclassified ACR 2 (benign). If it evolves, a biopsy is performed.
Upfront biopsy is also possible if the patient is anxious or if the lesion is too ambiguous for surveillance.
ACR 4 means suspicious finding (cancer probability between 2% and 95% depending on subtype 4a, 4b, 4c). ACR 5 means highly suggestive of cancer (>95%).
In both cases, biopsy is mandatory. If the lesion is also visible on ultrasound: ultrasound-guided biopsy at the office. If only visible on MRI: MRI-guided biopsy, in dedicated radiology, under local anesthesia.
ACR 4 doesn't mean breast cancer: most ACR 4a biopsies come back benign. The biopsy decides.
Ideally between day 7 and day 14 of the cycle (second week), when breast tissue is more "quiet" and the images are more reliable.
For postmenopausal women not on therapy, timing doesn't matter. On hormone replacement therapy, a few weeks off may be advised before MRI.
The radiology center will ask the date of your last period before scheduling.
MRI uses no X-rays and delivers no radiation, unlike mammography or CT.
The main contraindications concern incompatible metallic implants: older pacemakers, defibrillators, neurostimulators, certain metal foreign bodies. A safety questionnaire is filled in before every exam.
The contrast agent is generally well tolerated. Pregnancy is a relative contraindication.
Several solutions exist and claustrophobia is rarely a deal-breaker.
— You lie face down, which changes the perception of confinement.
— Mild anxiolytic premedication can be prescribed.
— Some centers have wide-bore or open machines.
— An alert button is in your hand.
If MRI remains impossible, contrast-enhanced spectral mammography (CESM) is the closest alternative.
Women carrying a BRCA1 or BRCA2 mutation have a significantly increased lifetime risk of breast cancer, often at a young age (before 40). At that age, breasts are dense and mammography sensitivity is limited.
Breast MRI is the most sensitive exam to detect early cancer in young women.
Discussion of prophylactic mastectomy is a separate topic, addressed in a dedicated consultation.
The three exams are complementary, not competing.
Mammography is the reference exam for breast cancer screening from age 50 in the organized screening program, and the baseline exam for any breast finding.
Breast ultrasound complements mammography in young or dense-breasted women, and helps characterize findings (cyst vs solid nodule).
MRI is reserved for specific situations: high familial risk (BRCA), breast cancer staging, ambiguous findings, implant surveillance.
The images are available right away on a CD or digital platform. The radiologist's written report is generally available within 24 to 72 hours, sometimes the same day.
Breast MRI is a long read requiring time: hundreds of images need analysis.
If a lesion is found that requires fast assessment, the radiologist will contact your prescribing physician directly.
Comparison with previous exams is one of the most powerful diagnostic tools. A lesion that has been stable over years is almost always benign. A new or changing area between two MRIs must be investigated.
The radiologist also compares your MRI with your recent mammography and ultrasound. Bring all your previous reports and images.
Not systematically. Standard follow-up after breast cancer mainly relies on annual mammography, with ultrasound as needed.
MRI is added in specific situations: young patient, dense breasts, history of lobular carcinoma, BRCA mutation, uninterpretable standard imaging, or in case of a worrying symptom.
After lumpectomy, MRI can help distinguish a scar from a recurrence in case of doubt.
A consultation to discuss your breast MRI report, understand your options, or get a second opinion — feel free to book an appointment.