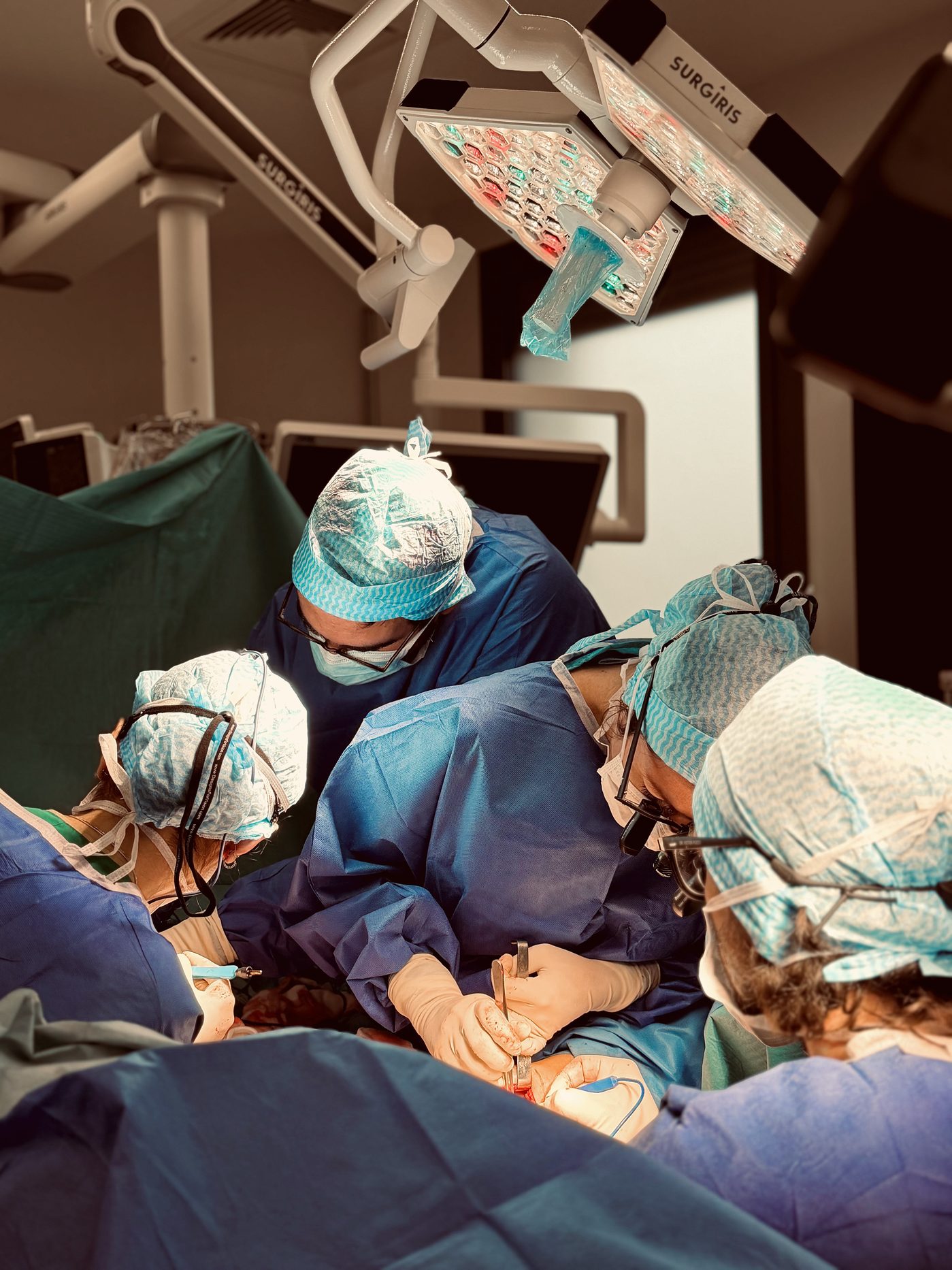
The procedure involves dissecting a horizontal ellipse of skin and fat from the infraumbilical abdominal region. The flap is harvested with an artery and a vein — the deep inferior epigastric perforator vessels — but without the rectus abdominis muscle or its fascia, which are carefully preserved.
The flap is then transferred to the chest. Its vessels are reconnected under a microscope to vessels of the axilla or chest: this microsurgical step keeps the tissue alive. Dr Zeitoun does not perform microsurgery himself — this part of the procedure is carried out in close collaboration with an experienced plastic microsurgeon. The flap is then shaped to rebuild a natural breast, without any prosthetic material.
The reconstructed breast is definitive and evolving: it follows weight fluctuations and the effects of gravity like a natural breast. The improved abdominal silhouette (tummy tuck effect) is often perceived as a bonus.
3–5 h
Operative time
A long procedure given the microsurgical time. The outcome is more natural and more stable over time than with any other technique.
100%
National health insurance base (ALD)
Procedure reimbursed based on the Sécurité Sociale tariff. Dr Zeitoun practises under sector 2 — additional fees apply. A written quote is provided before any surgery.
3–5 nights
Hospital stay
Daily microsurgical monitoring of the flap. Full recovery 4 to 6 weeks. Abdominal compression garment to be worn for several weeks.